Get Healthy!
Staying informed is also a great way to stay healthy. Keep up-to-date with all the latest health news here.
08 May
Ultra-Processed Foods May Speed Up Early Signs of Parkinson’s Disease, Study Finds
In a new study, people who consumed the highest amounts of ultra-processed foods were more likely to show earlier signs of prodromal Parkinson’s disease, the stage of the disease seen before tremors begin.
07 May
Teen Use of Nicotine Pouches on the Rise
A new study finds more high schoolers are using nicotine pouches -- alone and in combination with e-cigarettes.
06 May
Eating Nuts, Seeds and Corn Won’t Raise Your Risk for Diverticulitis, a Common Digestive Disorder
A new study finds no link between nuts, seeds and corn and diverticulitis risk in women. However, following a healthy diet was associated with lower odds of the painful disease.
I. Edwards HealthDay Reporter May 8, 2025
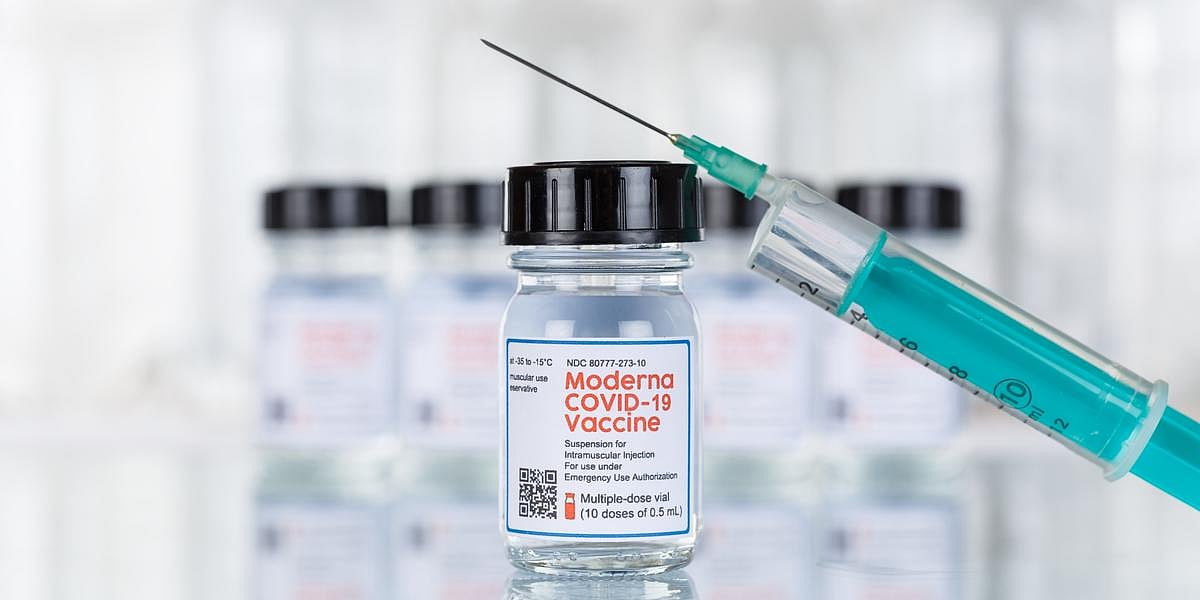
Moderna's Combo Flu and COVID Shot Shows Promise
THURSDAY, May 8, 2025 (HealthDay News) — A new vaccine that combines flu and COVID-19 protection in one shot shows promising results, but the U.S. Food and Drug Administration (FDA) says it wants more data before it can be approved.
Moderna researchers reported that the combo shot produced a stronger immune response against COVID-19 ... Full Page
I. Edwards HealthDay Reporter May 8, 2025
When Statins Aren't Enough, This Drug May Help Lower 'Bad' Cholesterol
THURSDAY, May 8, 2025 (HealthDay News) — A new drug combo lowers "bad" LDL cholesterol for people whose levels remain high even after taking statins.
The new pill pairs a new drug called obicetrapib with an existing one, ezetimibe. In a Phase 3 clinical trial, this combo reduced LDL levels by nearly 49% over about three months, accor... Full Page
I. Edwards HealthDay Reporter May 8, 2025
Trump Administration Ends CDC's Key Infection Control Committee
THURSDAY, May 8, 2025 (HealthDay News) — A federal committee that helped set national rules for infection control in hospitals has been shut down, raising concerns from health experts.
The Healthcare Infection Control Practices Advisory Committee (HICPAC) was terminated March 31, though members weren't told until early May, according... Full Page
Dennis Thompson HealthDay Reporter May 8, 2025
Face Mask Can Detect Kidney Disease Via Breath
THURSDAY, May 8, 2025 (HealthDay News) — Wearing a face mask to protect others from infectious disease continues to be hotly debated in the United States.
But what about wearing a face mask to detect chronic kidney disease?
A modified surgical face mask containing a specialized breath sensor can accurately detect when someone h... Full Page
Dennis Thompson HealthDay Reporter May 8, 2025
Worried About Prostate Cancer Screening? New Study Shows Better Judgment In Treatment
Some men would rather skip screening for prostate cancer due to fears that they’ll be rendered impotent or incontinent from cancer surgery.
But new research says those fears are unwarranted, thanks to improvements in the way doctors approach prostate cancer.
The number of unnecessary surgeries to treat low-risk prostate cancer ... Full Page
Dennis Thompson HealthDay Reporter May 8, 2025
Down Syndrome Patients Have Higher Stroke, Heart Attack Risk
People with Down syndrome have a much higher risk of stroke than people without the genetic disorder, a new study says.
Down syndrome patients have a 5.14 times higher risk of a stroke caused by a brain bleed, and more than 4 times higher risk of a stroke caused by a blood clot, researchers reported May 7 in the Journal of Internal Med... Full Page
Dennis Thompson HealthDay Reporter May 8, 2025
Early Alzheimer's Testing Can Provide Peace Of Mind
THURSDAY, May 8, 2025 (HealthDay News) — Knowing your risk for Alzheimer’s disease can provide peace of mind, but also might contribute to complacency regarding your overall health, a new study says.
People who underwent brain scans to learn their Alzheimer’s risk experienced less anxiety, even if the results showed highe... Full Page
Dennis Thompson HealthDay Reporter May 8, 2025
Ultra-Processed Foods Linked To Parkinson's Disease Risk
Fast food and ready-made packaged eats could be doing slow damage to people’s brains.
Ultra-processed foods like breakfast cereals, soft drinks, hot dogs and ketchup appear to increase a person’s risk of developing Parkinson’s disease, a new study says.
People who ate about 11 servings of ultra-processed foods per d... Full Page
Dennis Thompson HealthDay Reporter May 8, 2025
Sleep Apnea Linked To Memory-Related Brain Decline
Sleep apnea could be costing you brain power and increasing your risk of dementia and Alzheimer’s disease, a new study says.
The drop in blood oxygen levels that occurs during a sleep apnea episode appears to be linked to degeneration of brain regions associated with memory, researchers reported May 7 in the journal NeurologyFull Page
I. Edwards HealthDay Reporter May 7, 2025
Dr. Vinay Prasad to Head FDA Vaccine, Biologics Division
WEDNESDAY, May 7, 2025 (HealthDay News) — The U.S. Food and Drug Administration (FDA) has chosen Dr. Vinay Prasad, a professor at the University of California-San Francisco, to lead its Center for Biologics Evaluation and Research.
The division oversees vaccines and biologic medicines, including gene therapies, CNN rep... Full Page
I. Edwards HealthDay Reporter May 7, 2025
Top FDA Inspection Official to Retire Amid Staff Frustration
WEDNESDAY, May 7, 2025 (HealthDay News) — The official in charge of federal food and drug safety inspections will retire May 14.
Michael Rogers, associate commissioner for inspections and investigations at the U.S. Food and Drug Administration (FDA), announced his decision Monday in an email to colleagues.
"I have decided... Full Page
Carole Tanzer Miller HealthDay Reporter May 7, 2025
Europe Launches $565 Million Campaign to Attract U.S. Scientists
WEDNESDAY, May 7, 2025 (HealthDay News) — The European Union is looking to capitalize on the Trump administration's dismantling of U.S. research programs to beef up its own.
A $565 million program unveiled Monday aims to make "Europe a magnet for researchers," Ursula von der Leyen, president of the European Commission, said. Full Page
I. Edwards HealthDay Reporter May 7, 2025
Food Choices Could Influence First Period, Research Shows
WEDNESDAY, May 7, 2025 (HealthDay News) — What your child eats could play a role in when they start puberty, a new study shows.
Researchers found that girls who ate more inflammatory foods were 15% more likely to get their first period in the next month. On the other hand, a healthier diet lowered the odds by 8%. The findings were pu... Full Page
Dennis Thompson HealthDay Reporter May 7, 2025
Nicotine Pouch Use Doubles Among U.S. High Schoolers
The use of nicotine pouches nearly doubled among U.S. high school students between 2023 and 2024, a new study says.
These pouches, inserted between the gum and lip, provide teenagers an opportunity to use nicotine in a discreet, easily concealed way, researchers said.
About 5.4% of teens said they used nicotine pouches in 2024, compa... Full Page
Dennis Thompson HealthDay Reporter May 7, 2025
Conversion Therapy Harms Heart Health
Conversion therapy might harm a young person’s long-term heart health, a new study says.
Young adults assigned male at birth were nearly three times as likely to be diagnosed with high blood pressure if they’d been exposed to conversion therapy, a discredited practice that attempts to alter a person’s sexual orientation o... Full Page
Dennis Thompson HealthDay Reporter May 7, 2025
Stress Quadruples Risk Of COPD Flares, Study Says
WEDNESDAY, May 7, 2025 (HealthDay News) — Stress can make it even worse for people to deal with chronic obstructive pulmonary disease, or COPD, a new study says.
High levels of perceived stress are associated with a quadrupled risk of moderate or severe COPD flare-ups (excerbations), researchers reported recently in the Journal o... Full Page
Dennis Thompson HealthDay Reporter May 7, 2025
Shingles Vaccine Could Protect Heart Health
WEDNESDAY, May 7, 2025 (HealthDay News) — The shingles vaccine has benefits that stretch beyond protecting older adults from the painful skin condition, a new study says.
Folks who get the shingles jab have a 23% lower risk of health problems like stroke, heart failure and heart disease, researchers reported May 6 in the European... Full Page
Dennis Thompson HealthDay Reporter May 7, 2025
Childhood High Blood Sugar Can Cause Heart Problems In Young Adults
Persistently high blood sugar among teenagers can lead to heart disease by young adulthood, a new study says.
Teenagers had up to three times the risk of developing a heart condition called left ventricular hypertrophy if their blood sugar remained persistently high between ages 17 to 24, researchers reported recently in the journal Di... Full Page
I. Edwards HealthDay Reporter May 6, 2025
Salmonella Outbreak in 6 States Tied to Backyard Poultry, CDC Says
TUESDAY, May 6, 2025 (HealthDay News) — A salmonella outbreak tied to backyard poultry has made at least seven people sick across six states, U.S. health officials reported Monday.
The U.S. Centers for Disease Control and Prevention (CDC) said two cases were found in Missouri and one each in Florida, Illinois, South Dakota, Utah and ... Full Page
Dennis Thompson HealthDay Reporter May 6, 2025
COVID Boosters Might Not Be Updated For Next Season, FDA Commissioner Says
The head of the U.S. Food and Drug Administration (FDA) reiterated Tuesday that the agency is applying a more skeptical approach to this year’s round of COVID-19 vaccine boosters.
Companies applying for approval of COVID boosters are being encouraged to use “gold standard science,” including full-fledged clinical trials i... Full Page